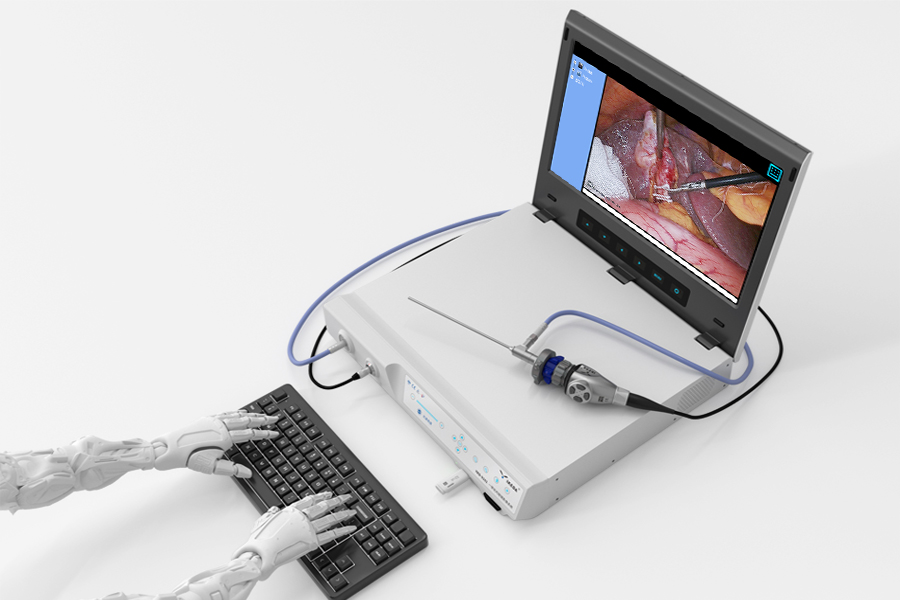
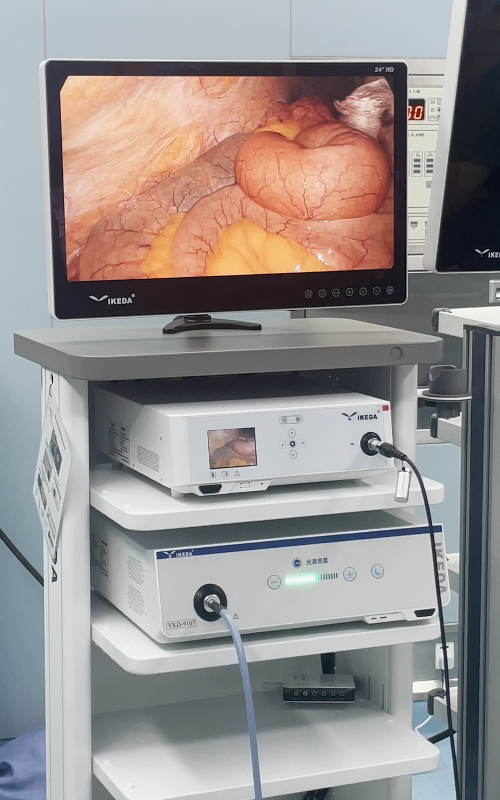
 Trap 1: "Idealistic Expectations"
Trap 1: "Idealistic Expectations"
Initially, the difficulty of gallbladder removal seems minimal. Mesentery-type and free-type gallbladders are even easier to remove than appendices, and these simpler cases are typically handled laparoscopically. What remains for open surgery are cases of chronic cholecystitis, suppurative or gangrenous cholecystitis, and the perilous atrophic cholecystitis, often termed a death trap.
Facing the gallbladder with these idealistic expectations can unknowingly lead you into a self-created mental trap.
Trap 2: Intrahepatic Gallbladder
Feeling pleased to have encountered a small gallbladder might be premature if it turns out to be an intrahepatic gallbladder. Before starting the removal, press the sides of the gallbladder with two fingers. If it sinks into the liver, congratulations—you have an intrahepatic gallbladder.
Surprised and caught off guard, aren't you?!
Trap 3: Gallbladder Infundibulum
From the outside, the infundibulum may look like a gradually tapering funnel. Perhaps due to our habit of drawing the gallbladder in this shape, we come to believe it really is funnel-shaped.
In reality, it often bulges towards the liver. Whether performing antegrade or retrograde dissection, when you reach the infundibulum thinking you are close to success, you may find its direction pointing towards the liver!
At this point, you realize that the gallbladder bed is a significant challenge, with the infundibulum being the toughest part. However, if you first open the peritoneum above and below the infundibulum, use a large curved clamp to separate it from the gallbladder bed, and pass a shoelace through the tunnel, gently lifting it reveals that this bulge is actually a perfect stepping stone!
Trap 4: Electrocautery for Hemostasis
When separating the gallbladder bed, bleeding from penetrating blood vessels is common. To quickly address this, aggressive electrocautery might be used. While generally effective, it can sometimes cause more severe bleeding. Look closely—the electrocautery might penetrate the gallbladder bed and enter the liver!
Trap 5: Variable Thickness
In cases of severe suppurative cholecystitis, the gallbladder wall is very thick, leading to the assumption that all parts are equally thick. However, during dissection, you might accidentally cut through the wall. Remember, the anterior and posterior walls of the gallbladder have different structures, varying in thickness and strength.
Trap 6: "Lost and Can't Return"
After cutting through the gallbladder wall, you might want to return to the normal layer quickly. Despite the edge of the breach being in sight, lifting it carefully might reveal that the previously sturdy gallbladder wall now tears like tofu skin, becoming increasingly unclear. As you struggle with this, inserting your finger into the infundibulum to find the correct direction might reveal the base pointing towards the hepatic hilum. A shoelace tied to the infundibulum can then become a lifeline!
Trap 7: "So Close Yet So Far"
For gallbladders with unclear cystic triangles, retrograde dissection is often considered. After painstakingly following the infundibulum to the hepatic hilum, you might find that your goal is tantalizingly close, yet frustratingly out of reach!
Trap 8: Sentinel Lymph Node
The sentinel lymph node in the cystic triangle helps identify the cystic duct and artery. However, in cases of severe inflammation, the enlarged sentinel lymph node can be problematic. Removing it is fine, but if curiosity leads you to cut it open, discovering a stone inside can be quite surprising!
Death Trap: Atrophic Cholecystitis!
A walnut-sized gallbladder may seem harmless, but have you considered it might not have always been that small? If the gallbladder bed, liver, hepatic hilum, cystic duct, common bile duct, cystic artery, and right hepatic artery are all shrunken into a walnut-sized space without gaps, would you still feel confident tackling it in one go?
Ultimate Trap: Cholecystostomy!
Given its fearsome reputation, avoiding cholecystectomy might seem prudent if your skills aren't up to par. However, severe cholecystitis, potentially leading to necrosis and perforation, necessitates intervention. An intermediate solution is cholecystostomy. But consider this: if inflammation has closed the cystic duct, the gallbladder continues to secrete mucus. Disconnecting it from the bile ducts leaves the gallbladder isolated. While inserting a tube is easy, explaining why it can't be removed is another story. Therefore, cholecystostomy should be a last resort, only when the patient's condition leaves no other option.
Gallbladder Removal Surgery — How to Choose
- Open Surgery or Laparoscopy? For highly skilled laparoscopic surgeons, most gallbladder removals can be done laparoscopically. However, for cases with recurrent bile duct infections, acute cholecystitis, atrophic cholecystitis, a history of upper abdominal surgery, suppurative cholangitis, bleeding disorders, obstructive jaundice, etc., open surgery is preferable.
- Subcostal Oblique Incision or Rectus Abdominis Incision? The benefits of an oblique incision include lower tension, smaller scars, better exposure of the hepatic hilum, and less postoperative adhesion. The drawbacks are significant damage to abdominal wall nerves and blood vessels, higher risk of infection, and the need for specialized instruments. In practice, the oblique incision is primarily used for minimally invasive small-incision cholecystectomy and cases requiring liver lobe resection.
- Antegrade or Retrograde Removal? The standard method is antegrade removal, which involves first freeing the cystic triangle, ligating the cystic duct and artery—essentially starting with the hardest part. Retrograde removal begins with the easier parts, hoping that a path will emerge as the surgery progresses. However, since the cystic artery is not initially dealt with, bleeding is more common, and freeing the gallbladder bed becomes challenging. Stones in the gallbladder can also be pushed into the common bile duct, creating new complications. Due to bleeding and traction, the anatomical relationships in the cystic triangle can change, making the procedure even harder. Once the gallbladder is partially freed, there's no turning back. But starting with the cystic triangle isn't always easy, especially with an enlarged infundibulum and hepatic hilum involvement. Alternatively, one can start from the middle, from the upper edge of the gallbladder, if the cystic triangle is difficult to free. In challenging cases, freeing the common bile duct and hepatic artery might be feasible.
- Ligate or Immediately Cut? After freeing the cystic triangle, it's tempting to immediately ligate and cut the cystic duct and artery. However, anatomical variations are common; the assumed cystic artery could be an aberrant right hepatic artery, or the cystic duct could have an accessory hepatic duct attached. Therefore, the cystic artery should be traced towards the gallbladder to confirm it solely enters the gallbladder before ligating and cutting it. After ligating the cystic duct, do not cut it immediately; wait until the gallbladder bed is fully freed, then cut it last. It might seem like extra effort, but like the flag in a golf hole marking the target, it provides a clear goal and direction. Without a clear target, the journey is the longest.